Skin is the protective barrier of our body. Even after the test of radiation therapy, we can make it tough again.
Dear skin cancer recovery partners, I’m in the follow-up clinic today. Again, I see a patient holding a pathology report, frowning, asking only one question: "Is it early or late?"
Wrong. Staging alone, not enough. Look at molecules.
From a professional perspective, many of you make this mistake. You glance at the final conclusion, skip the rows of indicators below—HER2, PD-L1, Ki-67—and miss the most important guide for precise treatment. These indicators, not just staging, decide whether you are suitable for targeted therapy or immunotherapy, directly affecting your prognosis.
I’ve been in this field for 30 years. Too many patients, because they didn’t understand these indicators, missed the best treatment opportunity. That’s why I feel I must teach you to "read" your own report.
Challenge? Big. At first, I tried to explain. "PD-L1 is a protein on tumor cells..." Before I finished, the patient shook their head. "Doctor, you decide. I don’t understand these big words."
Wait, patient怎么 only look at staging? HER2 positive, they don’t know?糟了, did I not explain clearly?
I rubbed the calluses on my hands—formed from years of operating medical equipment—sighed. Staring at the pathology report on the desk, my glasses slipped down my nose. I pushed them up, determined to find a way.

I designed a "three-step method to read pathology reports": first look at the type, then the grade, finally the molecular markers. Simple, right?
Let me put it plainly. HER2, it’s like the accelerator of cancer cells. Positive means the accelerator is stuck. But we have targeted drugs—like trastuzumab—to hit the brake. For skin cancer patients with HER2 positive, using this drug can increase the 5-year survival rate by 30%.
PD-L1, think of it as a "shield" on tumor cells. High expression means the shield is strong, and immunotherapy can break this shield, letting your own immune system attack the tumor. Low expression doesn’t mean no hope—there are other combination therapies.
Ki-67, it reflects how fast cancer cells multiply. The higher the index, the more active the tumor. It helps us judge how aggressive the cancer is and choose the right treatment intensity.
I was explaining this to a patient last month. Just as I said "Ki-67 index over 30% means..." Suddenly—wait, the nurse knocked, the next patient arrived. I paused, apologized, and when I came back, the patient leaned forward. "Doctor, continue. I want to understand my report."
That’s the turning point. I made a visual guide, with simple drawings of accelerators and shields, marked the key indicators with red pens. Gradually, more patients started asking: "What’s my PD-L1 expression?" "Is my HER2 positive?"
I remember the first patient who fully understood HER2. A 52-year-old woman with skin cancer. After reading her report, she took the guide I made, pointed to the HER2 positive mark, and said: "So I can use that targeted drug? That’s good news." Later, her treatment effect was excellent—her skin lesions gradually healed, and she regained confidence.
Your skin records your bravery, and I am here to heal its wounds.
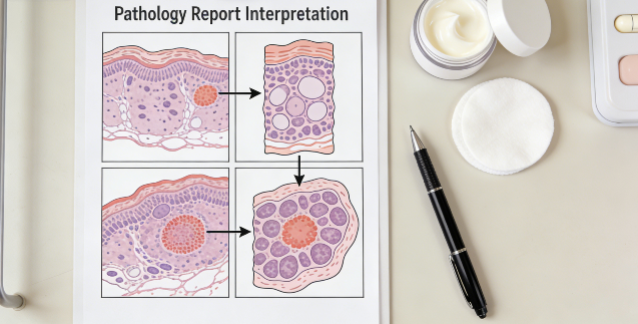
From a professional perspective, let’s talk about the standard interpretation process. First, confirm the histological type and grade—this tells you what kind of skin cancer it is and how severe it is. Then, check the immunohistochemistry results—that’s where HER2, PD-L1, Ki-67 are. Finally, combine molecular testing results to make a comprehensive judgment.
Please note, two pitfalls to avoid. First, never judge prognosis only by staging. Molecular typing is often more important. A patient with late stage but PD-L1 high expression may have a good effect with immunotherapy. Second, don’t give up because of "bad indicators". Modern precision medicine has many drugs targeting specific targets—there’s always hope.
I was recording medical advice this morning. Holding the pen, the calluses on my fingers rubbed against the paper, a little stinging. But I kept writing, making sure every indicator explanation was accurate. Suddenly, the computer froze. I restarted it, and when I came back, my train of thought was clearer.
Now, more and more patients can actively participate in treatment discussions. They understand that knowledge is power—reading the report is the first step in cooperating with doctors in treatment.
I printed out the pathology report interpretation guide, just about to hand it to the patient in front of me. Wait, I found a new indicator not marked on the guide. I picked up the pen, pressed the tip lightly, ready to add it quickly.
Take good care of your skin—it will stand with you to beat cancer.


